Doctors for Doctors
16 Jun 2020
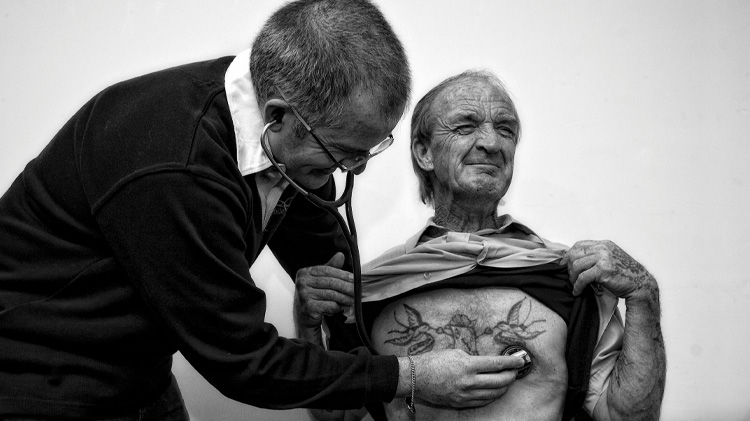
In 2008, I started Homeless Healthcare with a colleague. From an office in my house, we planned to visit drop-in centres twice a week to provide health care to people experiencing homelessness. Our biggest mistake was underestimating the demand – within three months it became a full-time job.
After years of domestic violence, John’s mother and father separated when he was eight years old. John and his family moved to rural Western Australia with his new stepfather. It’s at this point that John felt his life changed forever. His stepfather hit him the next day when he was being naughty. This gradually increased, and after a while John didn’t even misbehave before he was hit – and the regular hitting turned into regular beatings.
To make things worse, John’s stepfather sexually abused him when he was 12 years old. After this happened for the fourth time, John ran away to Perth. Having no other family in Australia, he was forced to live on the streets. Starving, he started eating leftovers in food courts and rubbish bins.
Eventually he fell in with some older boys living on the streets. They introduced him to cannabis, and he found it helped him relax and sleep better. It wasn’t long until he was using this and other drugs on a regular basis.
At the age of 17, John had his first episode of depression. Not knowing what was going on, he didn’t seek professional help. When he was 23 years old, he went to the Emergency Department (ED) when manic and was told by the doctor that it was ‘just the drugs’.
Left untreated, John continued to self-medicate with illicit drugs. He eventually caught hepatitis C from IV drug use and developed chronic obstructive airways disease from heavy smoking.
Still homeless and in his early 40s, John saw a GP for the first time in 2012.
Eight years later, John continues to see our service regularly. He takes his mood-stabilising medication regularly. Now housed in a Department of Housing property, he has re-engaged with his two teenage children who enjoy coming over for sleepovers. His latest aim is to walk more steps each day than his doctor, and is losing weight steadily.
Tri-morbidity (co-existing mental health, drug and alcohol problems, and physical health problems) occur in more than half of the people experiencing homelessness. As a result, they have a life expectancy of approximately 47 years.
Our service recognised that the lack of safe and secure housing was at the core of a homeless person’s poor health – so we would need to work closely with the agencies that help find housing.
Homeless Healthcare now employs over 40 people. We provide general practice clinics in drop-in centres, a drug and alcohol rehabilitation service, transitional accommodation services, and domestic violence shelters – all from an office in West Leederville.
In 2016, we established an in-reach program at Royal Perth Hospital five days a week for patients presenting to the ED identified as homeless, and an after-hours service to support those who’ve been rehoused. The program was aimed at alleviating the increasing demand homelessness places on Perth’s emergency services. Since implementation, the number of patients presenting to the ED has dramatically decreased.
We’re always looking for medical staff who have that extra bit of compassion. As a not-for-profit organisation, we also rely on donations to continue our work.
If you’re interested in joining us on our mission, please email generalmail@hhc.org.au, call 08 6260 2092, or visit our website homelesshealthcare.org.au.
- It's estimated that more than 100,000 people are homeless on any one night in Australia.
- Homeless Healthcare has treated close to 10,000 individuals since its launch, with approximately 2,800 last year.
- Practitioner visits to Homeless Healthcare continue to grow (1,500 in 2011 to 14,000 in 2018).
Professional boundaries in healthcare - Part 1
Boundaries with patients present in numerous ways every day and all health practitioners
11 Aug 2025
Understanding Professional Medical Indemnity Insurance
Do you understand the ins and outs of professional medical indemnity insurance?
11 Aug 2025
Professional boundaries in healthcare - Part 2
Boundaries with patients present in numerous ways every day and all health practitioners
11 Aug 2025
Understanding Voluntary Assisted Dying laws
What are the laws and processes in place for VAD and what is my role?
22 Jul 2025






