Non-Invasive Prenatal Testing – Ethical & Medico-legal Issues
15 Nov 2017
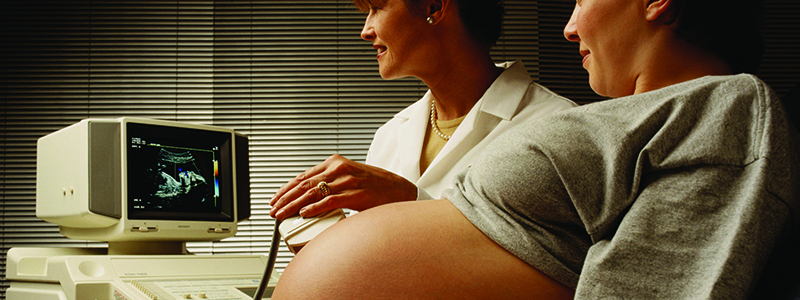
This is a problem with aneuploidy screening. Increasingly the tests being performed reflect a push by industry, rather than a careful, scientific and ethical analysis of the potential implications of newly available testing.
Previously, pregnant women were offered invasive diagnostic testing for Down syndrome, the most common genetic cause of intellectual handicap, on the basis of advanced maternal age. Women aged 35-37 and above were counselled that the risk of pregnancy loss was roughly comparable to their age-related risk of Trisomy 21, and offered amniocentesis or chorionic villus sampling (CVS).
Over the past 40 years, there have been significant changes in the prenatal aneuploidy screening options available, coupled with substantial improvements in the performance of available screening tests. This has led to the current universal, rather than selective, offering of aneuploidy screening in pregnancy.
We have moved closer to the “perfect” test – one with detection rates of 100% and risk of 0%. But the old “Triple test” also allowed for early diagnosis of neural tube defects. First trimester screening, involving biochemical testing and nuchal translucency measurement from 11-14 weeks, offered higher rates of Trisomy 21 diagnosis and other useful information, including early detection of major anatomical anomalies, and insight into possible third trimester complications like intra-uterine growth restriction and pre-eclampsia.
Non-invasive prenatal testing (NIPT)
Recent Australian publications have demonstrated an increase in the prenatal detection of Trisomy 21 at the same time as a decline in invasive testing.1,2 This trend was occurring prior to the 2012 introduction of NIPT. However, it has accelerated with MBS data showing a 53.7% reduction in amniocentesis and CVS over the past five years.2
NIPT for maternal plasma cell-free DNA is a high-level screening test for Trisomy 21 (sensitivity 99.3%), Trisomy 18 (97.4%) and Trisomy 13 (97.4%).3 The positive predictive value (PPV) – the probability that those who have a positive test actually have the condition – is highest in high risk populations.
Virtually all new medical innovations exhibit an initial enthusiasm, followed by tempering of the optimism, and then a plateau into realism as the true benefits and concerns become evident. NIPT is no exception to this. It is the most sensitive and specific test available for Trisomy 21 in both high and low risk populations. However, it remains a screening test, meaning there is an imperative for confirmatory diagnostic testing. Of huge concern is that women are proceeding directly to termination of pregnancy following an abnormal NIPT result without confirmatory karyotyping.4
NIPT has been marketed as providing increased safety, accuracy, and availability at an early gestation. However, its performance characteristics vary substantially with the prevalence of the condition studied. NIPT has also been introduced into Australia with no government subsidy, creating a dichotomy in test provision, based on means to pay rather than clinical need.
The biotechnology companies who have invested billions of dollars into research and development have driven the market, not doctors. The companies have elected what genetic conditions to test for, raising significant concerns about the “expanded NIPT panel” and testing for sex chromosome abnormalities (SCA) by several professional societies and individual doctors.
The impact on human life
Human life is the core business of medical practitioners. We exist to prevent, ameliorate or cure disease. A core function of antenatal care is the timely detection of significant fetal malformations to provide parents with options for ongoing care, which may include termination for severe fetal conditions. While some women would never consider it, many others elect to interrupt their pregnancy following the diagnosis of a severe fetal condition. There is evidence that the earlier an abnormal fetal condition is diagnosed, the higher the termination rate.
The emergence of NIPT raises several ethical issues for doctors, patients and society. It has been marketed commercially, with practitioners concerned that failing to recommend the test may be perceived as sub-optimal care, opening up medico-legal or reputational risk. It has been marketed as a universally positive development in antenatal care, with little discussion about an alternative view.
Many women and healthcare providers now view NIPT as a routine component of obstetric care, and this may result in women feeling pressured to have testing. Some have made the analogy of NIPT as a screening test with that of prenatal ultrasound, a testing modality for which informed consent is usually conspicuously absent and is now in almost universal use with no general perception of performance characteristics or risk.5
Indeed, some doctors view informed consent for NIPT as unimportant, perceiving it as having no direct risk to the fetus.6 Recent data has suggested that women value the perceived safety of NIPT more than the information it provides.7 It is very clear that pre-test counselling for NIPT, including test performance characteristics, limitations, risks, and the potential for unanticipated information is required, but this adds a significant time burden.
Medico-legal pressures may influence the use of NIPT. Fear of a complaint or claim for failing to recommend NIPT may increase its use, a phenomenon well recognised in modern medicine where litigation concerns alter practice, especially in regards to use of laboratory and imaging modalities.
However, there are concerns by some doctors that the benefits of NIPT have been overstated and the disadvantages largely suppressed. As the use of NIPT increases, the potential harms are emerging. Test failure, typically secondary to a low fetal fraction, is more common than initially believed, and may lead to long delays in obtaining results.
Ethical issues such as early sex determination and detection of SCAs are controversial. Most companies now routinely offer sex chromosome testing as a component of NIPT. Concerns have been raised that determination of fetal gender at early gestations may lead to termination if the gender is not to the parents’ liking.
SCA such as Monosomy X, 47,XXY, 47,XYY and 47,XXX have typically been detected previously as a result of amniocentesis or CVS for other reasons (e.g. advanced maternal age). The SCA phenotypes are highly variable, and prior to NIPT there had been a decreasing trend of termination for these conditions. The most common reasons for termination are parental fear of abnormal child development and directive counselling.
It is important that doctors requesting NIPT carefully discuss with the patient the potential for detection of a SCA when fetal gender is being ascertained and the limitations of this aspect of the test. The patient can elect to include or not include testing for SCAs. NIPT performance for SCAs is much poorer than for Trisomy 21, typically with a sensitivity of 90%.8 In a recent publication from the USA that reviewed 2,851 pregnancies having NIPT by massively parallel sequencing techniques, the false positive rate of NIPT for Monosomy X was 91% (10/11 cases), i.e. a genuinely dismal PPV of 9% with no true positive cases in the presence of a normal nuchal translucency.9 With such a high false positive rate, routine screening for Monosomy X should be critically reviewed.
A medico-legal and ethical dilemma
New technology drives a tendency to test for an increasing number of abnormalities, but as a society we have yet to determine the conditions of offering prenatal screening. Industry is framing the testing agenda, rather than medical need or societal values. It is easy to fall into the data trap of prenatal testing, rather than considering the values of human life in its many forms.
Currently, prenatal screening and diagnosis focuses on clinically significant disorders with well recognised phenotypes for which early diagnosis offers benefits. NIPT is potentially a powerful tool in fetal genetic diagnosis – and the range of recognisable conditions needs to be carefully evaluated to ensure there is merit in their detection; that the performance characteristics are robust and accurate; and that the testing modalities operate within ethical principles.
It is essential for GPs, Obstetricians and other clinicians to provide accurate pre-test and post-test counselling. Explaining the possibilities and limitations of prenatal testing is complex and time consuming. It is incumbent to delve past “I want that new test where I can find out whether it’s a girl”. If poorly targeted, the new test can cause great angst and heartache for patients. It is also an area of emerging risk for doctors and the society they serve.
Prof Jan Dickinson
Professor of Maternal Fetal Medicine
University of Western Australia
Dr Michael Gannon
Head of Department, Obstetrics & Gynaecology
St John of God Subiaco Hospital
The views expressed in this article belong solely to the authors, and do not represent the views and opinions of MDA National.
References
- Hui L, Muggli EE, Halliday JL. Population-based Trends in Prenatal Screening and Diagnosis for Aneuploidy: A Retrospective Analysis of 38 Years of State-wide Data. BJOG 2016;123:90-97.
- Robson SJ, Hui L. National Decline in Invasive Prenatal Diagnostic Procedures in Association with Uptake of Combined First Trimester and Cell-free DNA Aneuploidy Screening. Aust NZ J Obstet Gynaecol 2015;55:507-510.
- Taylor-Phillips S, Freeman K, Geppert J, et al. Accuracy of Non-invasive Prenatal Testing Using Cell-free DNA for Detection of Down, Edwards and Patau Syndromes: A Systematic Review and Meta-analysis. BMJ Open 2016;6(1):e010002.
- Dar P, Curnow KJ, Gross SJ, et al. Clinical Experience and Follow-up with Large Scale Single-Nucleotide Polymorphism-based Non-invasive Prenatal Aneuploidy Testing. Am J Obstet Gynecol 2014;211:527.e1-17.
- Favre R, Moutel G, Duchange N, et al. What about Informed Consent in First-trimester Ultrasound Screening for Down Syndrome? Fetal Diagn Ther 2008;23:173-184.
- Van sen Heuvel A, Chitty L, Dormandy E, et al. Will the Introduction of Non-invasive Prenatal Diagnostic Testing Erode Informed Choices? An Experimental Study of Health Care Professionals. Patient Educ Couns 2010;78:24-28.
- Minear MA, Lewis C, Pradhan S, Chandrasekharan S. Global Perspectives on Clinical Adoption of NIPT. Prenat Diagn 2015;35:959-967.
- Gil MM, Revello R, Poon LC et al. Clinical Implementation of Routine Testing for Fetsl Trisomies in the UK NHS: Cell-free DNA Test Contingent on Results from First Trimester Combined Test. Ultrasound Obstet Gynecol 2016;47:45-52.
- Reiss RE, Discenza M, Foster J et al. Sex Chromosome Aneuploidy Detection by Non-invasive Prenatal Testing: Helpful or Hazardous? Prenat Diagn 2017;Mar 21. doi: 10.1002/pd.5039. [Epub ahead of print]
Professional boundaries in healthcare - Part 1
Boundaries with patients present in numerous ways every day and all health practitioners
11 Aug 2025
Understanding Professional Medical Indemnity Insurance
Do you understand the ins and outs of professional medical indemnity insurance?
11 Aug 2025
Professional boundaries in healthcare - Part 2
Boundaries with patients present in numerous ways every day and all health practitioners
11 Aug 2025
Understanding Voluntary Assisted Dying laws
What are the laws and processes in place for VAD and what is my role?
22 Jul 2025





