You Can Lead a Horse To Water…
04 Nov 2014

But – and there’s always a “but” – patients have the right not to take your advice. There may be no agreement on a way forward. In the same way that patients cannot demand treatment, you cannot impose it.
-
Sometimes they will explicitly and immediately refuse.
“I’m not going to/can’t do that. What else can you suggest?” -
Sometimes they will endlessly argue the point – or try to “trade”.
“If I run an extra 10km a week, can I still smoke five cigarettes a day?” - Sometimes they will apparently acquiesce, and then just not do it.
There’s enough medical paternalism left in all of us that we want to see our patients make “good” health decisions. We respect their right to make their own autonomous decisions but we do our best to motivate them to follow our advice.
So, how do you do that?
For a start, you need to ensure that the patient is fully informed about why you have recommended a particular course of action and what it entails. If this sounds like “informed consent”, that’s because it is. That concept applies to all treatments (and investigations) that we recommend, not just operations.
You should routinely discuss the risk of not following your advice. We live in an age where there is minimal tolerance of uncertainty and minimal tolerance of risk. Commonly we are asked, “Are you certain that what you suggest is safe?” to which the best reply is, “No – but I am certain that not doing it is not safe.”
The concept of having to accept some risk in order to prevent a greater risk is not welcome news. We need then to divert attention from comparing one risk to another to comparing the risk/benefit balance in various options. For example (and I’m not saying that the following statement is true) you might need to say that “Ibuprofen will bring down your temperature and relieve your pain better than paracetamol but it is more likely to cause indigestion than paracetamol.”
Similarly, we need to move the focus away from the pain incurred now in following our advice to the benefit which will accrue in the future if it is followed. The problem is that the benefit may not be appreciated as it is a probability, not a certainty – the patient probably won’t have a heart attack, probably won’t develop diabetes, etc. The certainty of pain now can only be balanced against the probability of benefit. That’s a hard sell!
“Tough love” can be a useful tool
P: “You’ll be very disappointed in me doctor.”
D: “Why?”
P: “Well you spent all that time explaining to me why I had to lose weight, and how to go about it, and here I am having lost no weight at all.”
D: “I appreciate how hard it is to lose weight. I’m concerned – for you – that you felt you couldn’t do what I suggested. But you’ll be the one that has the heart attack/stroke/get diabetes, not me. I’m satisfied that the advice I gave you was the right advice for you. What you do with that advice is entirely up to you. I hope though that when you think about how hard it is to lose weight, you also think about what could be the consequences to you if you don’t.”
Notice how the longer doctor statement starts with empathy (“I appreciate… I’m concerned…” and then moves to tension (“you’ll be the one…”, and the change is signalled by the word but.
Things to watch out for
Watch out for the “What about… Yes but” “game” first described by Eric Berne in his wonderful 1964 book Games People Play.1 (It’s well worth a read and a lot of it is available for free, online.)
For example, in recommending various strategies for losing weight, when you suggest cutting back on carbs the patient might say, “But when I do that I get hypo and very dizzy” or when you suggest a diet plan, the patient might say, “But I can’t cook a different meal every night for me and then for the rest of the family” and when you recommend exercise they might say, “But even walking hurts my knees.” That’s also called “clay pigeon shooting”. Every time you throw up a clay pigeon, they shoot it down.
Sometimes I explain the “What About… Yes but” game to the patient and say that I won’t play it. Let’s face it, there can’t be a person on this planet who doesn’t know how to go about losing weight. What’s lacking is the motivation to do what they know they should do. And motivating a patient is always a balance between empathy and tension. Too much empathy leaves the patient cosily making no change. Too much tension and the patient just switches off.2
“Tough love” is the best way to stop that game in its tracks:
“I hear what you’re saying but you need to lose weight.”
“The fact that losing weight is hard to do does not alter the very pressing need for you to do it.”
In short, because you can’t make the horse drink, you can motivate it to want to drink!
What should be discussed
- The advised treatment
- Possible alternatives
- Why the proposed treatment is recommended
- Benefits/risks of proposed treatment
- Benefits/risks of alternatives
- Risk of not following the advice
Empathy/Tension model for change
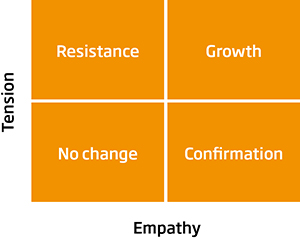
Adapted from Daloz 1986
References
1. Daloz, L. Effective Teaching and Mentoring. San Francisco: Jossey Bass, 1086.
2. Daloz, L. Mentor: Guiding the Journey of Adult Learners. Wiley: New York, 2012, p. 208.
Professional boundaries in healthcare - Part 1
Boundaries with patients present in numerous ways every day and all health practitioners
11 Aug 2025
Understanding Professional Medical Indemnity Insurance
Do you understand the ins and outs of professional medical indemnity insurance?
11 Aug 2025
Professional boundaries in healthcare - Part 2
Boundaries with patients present in numerous ways every day and all health practitioners
11 Aug 2025
Understanding Voluntary Assisted Dying laws
What are the laws and processes in place for VAD and what is my role?
22 Jul 2025






